Gingival recession means the gum tissue pulls back and exposes the tooth root. Knowing the gingival recession stages matters because each stage points to different treatment needs and likely outcomes. Staging helps your dentist or specialist decide whether monitoring and better home care will do, or if surgery, grafting, or implant-based reconstruction is needed. If you live locally, asking specifically about gingival recession stages in Scottsdale or gingival recession stages in Phoenix, AZ makes it easier to get care that matches available specialists and technology.
What Is Gingival Recession?
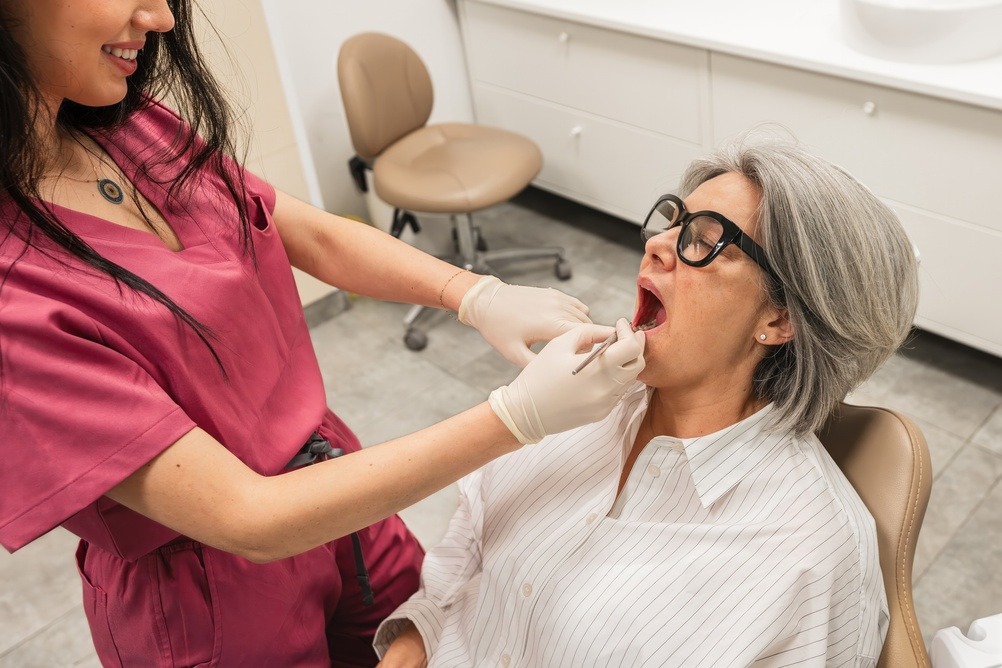
Gum recession happens when the gum edge moves away from the crown of the tooth and the root becomes visible. Roots are softer than enamel, so exposed roots are more likely to wear down, decay, and cause sensitivity. Recession can happen from long-term gum disease (periodontitis) or from mechanical forces like hard brushing. It is different from pocketing in gum disease — recession is loss of gum height, while pockets are deep spaces forming between tooth and gum from infection. Both can lead to tooth loss if untreated.
Common Classifications: Gingival Recession Stages
Dentists use staged systems to describe how much tissue is lost. Simple staging helps predict how successful treatment is likely to be.
Miller Classification (Class I–IV)
– Class I: Recession does not reach the gum line between teeth (no loss of interdental bone). Good chance for full root coverage with surgery. – Class II: Recession goes past the gum line but still no loss of interdental bone. Root coverage is generally achievable. – Class III: Recession beyond the gum line with some loss of bone or misaligned teeth between teeth. Partial root coverage may be possible. – Class IV: Severe tissue and bone loss with poor tooth alignment. Predictable root coverage is unlikely.
Cairo/RT Classification (RT1–RT3)
The Cairo system focuses on whether there is loss of attachment between the teeth rather than just visible recession. – RT1: Root exposure without loss of interproximal attachment — best chance for coverage. – RT2: Some interproximal attachment loss but not as severe as RT3 — partial coverage possible. – RT3: Significant interproximal loss — limited predictability. Some clinicians prefer Cairo/RT because it links directly to likely surgical outcomes.
Signs and Symptoms By Stage
Early stages often cause mild sensitivity to cold, hot, or sweet foods and a small notch near the gum line. As stages advance, more root surface becomes visible, sensitivity increases, and teeth may look longer. Later stages can lead to root decay, increased tooth mobility, and even tooth loss. At home, watch for longer-looking teeth, gum tissue that looks thin or pulled back, new gaps between teeth, or persistent sensitivity. Report these signs to your dentist right away.
Common Causes and Risk Factors
Periodontal (gum) disease
Bacterial infection destroys gum tissue and bone, causing gums to recede over time.
Mechanical trauma (toothbrush, toothbrushing technique, oral appliances)
Hard brushing, using a toothbrush with firm bristles, or incorrect technique can wear away gum tissue. Ill-fitting mouthguards or partial dentures can also cause localized recession.
Orthodontics, occlusion, and tooth position
Teeth pushed too far forward or with poor bite alignment may put pressure on the gum, making recession more likely.
Smoking, genetics, and age
Smoking reduces blood flow and healing, increasing recession risk. Some people inherit thinner gums that are more prone to recede. Recession also increases with age. These factors help explain how patients move through different gingival recession stages and why treating the cause is as important as treating the recession.
How Gingival Recession Stages Influence Treatment
Treatment follows a ladder based on stage and cause. Early stages often need better home care, a gentler brushing method, and regular cleanings. Moderate recession can respond well to minimally invasive root coverage procedures, like connective tissue grafts. Advanced stages with significant bone loss may need more complex grafting and regenerative surgery; sometimes extraction and implant-based restoration become the safest long-term option. Predictability is higher with early-stage recession; advanced stages may require combined surgical approaches and staged treatment planning.
Prevention and At-Home Care
– Use a soft-bristled toothbrush and gentle circular strokes. – Switch to a low-abrasion, desensitizing toothpaste if you have sensitivity. – Get routine dental cleanings and periodontal checkups. – If you grind or clench, ask about a night guard to protect gums and teeth. – Quit smoking to improve gum health and healing. Preventive steps can stop or slow early-stage recession; once tissue is lost, professional treatment is often needed to restore coverage.
When to See a Specialist
Seek prompt evaluation if you notice rapid recession, new or severe sensitivity, exposed roots with decay, or loose teeth. A periodontist treats gum tissue and grafting procedures. An oral surgeon or implant/restorative team becomes important if tooth loss or full-arch reconstruction is a possibility. Complex cases often benefit from a coordinated team approach.
About ProSmile Dental Implant Center
ProSmile Dental Implant Center serves Scottsdale and Phoenix, Arizona with a team-based model that combines surgical and restorative specialists. The practice uses 3D imaging, digital planning, an in-house lab, and advanced sedation to plan complex reconstructions when recession leads to tooth loss. With extensive implant experience and full-arch work, ProSmile offers coordinated options ranging from gum-sparing treatments to implant-supported restorations.
Next Steps: Getting Evaluated for Gingival Recession Stages
At a consultation expect an exam, measurements of gum attachment, and 3D or X-ray imaging if needed. Ask which gingival recession stages describe your condition, what caused the recession, and what outcomes you can expect with different treatments. Simple next steps may be improved home care and monitoring, referral to a periodontist, or a tailored treatment plan that includes grafting or reconstruction. If you notice any gum pulling back, sensitivity, or exposed roots, schedule an evaluation to protect your long-term oral health.